Help Desk FAQs
Frequently asked questions and answers from the CSW Help Desk
Continuing Education Requirements
details
ABN Usage Clarification
details
Patient Records
details
Leaving Practice
details
ICD-10 Codes
details
Medicare Documentation
details
Medicare Fee Schedule
details
Process for "Firing" a Patient
details
Purging Patient Files
details
HIPPA
details
Opting out of Medicare
details
Discounts, Cash and Credit Cards
Dry Needling
- A certification in dry needling is not necessarily required in order to practice dry needling in Wisconsin. The Chiropractic Examining Board after very long discussions made the decision that dry needling was always within the scope of practice of chiropractic and that going through rulemaking to achieve the incorporation of dry needling would not be necessary. The Board determined that there was no need for a requirement for specific education prior to performing the service. All board members agreed that the chiropractor must be trained and capable of performing the services similar to any service that a chiropractor would perform on a patient, but they did not require specific hours or courses to be taken prior to a chiropractor providing the services. Click here for the reference to the Board’s action.
- Billing? Delegation?
OIG Exclusion Database Search
(Office of Inspector General) OIG Exclusion Database Search Website: https://exclusions.oig.hhs.gov
Nutrition Certification Requirments
A Nutritional Certificate can be obtained by going through a 48-hour certification program. To maintain this certificate active, 4 hours of Nutritional CE must be completed each biennium.
Medicare PAR vs. Non-PAR
Chiropractors that see any Medicare patients must be enrolled with Medicare as providers.
They can elect to be participating or non-participating (“par” or “non-par”).
As a par provider, they can bill their regular, full fees for services. However, Medicare will only reimburse 80% of their “par amount” shown below. The patient is responsible for 20% of the par amount and any remaining deductible they have. Medicare will pay the provider directly (as an “assigned” claim).
As a non-par provider, the clinic can only bill up to their “limiting charge”, shown below. They may collect this fee upfront from the patient, or can wait for payment from Medicare (as an “assigned” claim). Either way, the provider must bill Medicare (with one exception, which is for another topic). Medicare will reimburse the patient 80% of the “non-par amount” shown below.
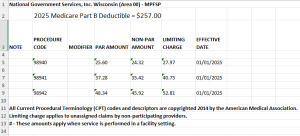
These fees are updated annually (and often more) in the last six weeks of the year and are posted on the MGS Medicare website.
Fill in Doctors
The best, and probably most efficient way to get temporary coverage is to reach out to “Doc For A Day”. Here is a link to their website: https://www.docforaday.com/
Off Sight Adjusting
There are a couple of things you should consider which we have listed below:
- Check with your MP carrier to make sure you are covered. Most do, but good to be sure
- Realize that the people you would be adjusting are now your patients and you have to follow all of the same procedures and policies that you currently follow in your office including:
-
- Obtaining a written history
- Performing a proper examination and recording the information
- Written informed consent
- Proper documentation. of your services
- Maintaining a proper DC/Patient relationship
-
- Other considerations are HiPAA procedures to follow as well as no surprises act information.
- For billing insurance there are specific “pointers” that you need to fill out to indicate the location of the services provided.
- You need to be aware of issues with Medicare/ Medicaid if anything “free” is offered
Hopefully this provides you with enough basic information to make an informed decision on how to proceed.
Informational Webinars
Legal Changes Involving Non-Compete Agreements - Webinar
The CSW is excited to launch a new series of webinars, seminars and programs aimed at increasing the success of our members. One key initiative is our Business Success Series, where top-level professionals will share insights on creating successful and compliant business practices.
To kick off the series, we are hosting a legal seminar related to the new non-compete rules that will significantly change employment agreements that have been in place for decades. Specifically, there are new business related rules that will dramatically change how chiropractic offices, especially those who have associates or are considering an associate agreement, conduct business.
The CSW always seeks out the best sources for our membership. As such, we are thrilled to announce that Attorney Brad Fulton will lead this webinar. Brad is a former managing partner of one of Wisconsin’s largest law firms and a top employment attorney with over two decades of experience assisting the chiropractic profession. In our opinion, his trial experience with chiropractic non-compete litigation makes him the best resource for understanding these new rule changes.
Medicare Documentation - Webinar - WPS Letters
The CSW’s team of Medicare experts have developed this presentation to provide Wisconsin DC’s an expansive review of required Medicare documentation to demonstrate both active treatment and maintenance care in Medicare and Medicare secondaries. The CSW has been receiving multiple calls related to the WPS letter that was sent out discussing changes for 2024. Please note that there is a very simple answer to this issue. Since the CSW has several Medicare experts within our member support team, we have developed this webinar to assist our members with a more expansive review of required Medicare documentation to demonstrate both active treatment and maintenance care in Medicare and Medicare secondaries.
Simple Answer:
The information provided in the WPS letter is both correct and not new. WPS is simply stating a policy that has been in existence for decades. Maintenance care has never been covered as a payable service. It appears that WPS has been incorrectly paying for services deemed maintenance and will be upgrading their systems to prevent this from happening in the future. The positive is that they have stated they would not be seeking payments based on the error.
What about the Wisconsin mandate?
The Wisconsin mandate does not obligate an insurance company, including a Medicare secondary, to pay for maintenance care. The Wisconsin mandate does assist with payments for services associated with Active Treatment, such as examinations, x-rays, and therapies. Once a patient is determined to be maintenance, then the insurance company policies dictate that no payments are required to be made. There may be a slight variance from the policy definitions of maintenance in Medicare secondary policies when compared to Medicare, but generally, once a patient is deemed maintenance by Medicare standards, they will very likely be deemed maintenance by Medicare secondary policies as well.
Corporate Transparency Act - Webinar
Updated Alert: 3/3/25
The U.S. Treasury Department is announcing today that, with respect to the Corporate Transparency Act, not only will it not enforce any penalties or fines associated with the beneficial ownership information reporting rule under the existing regulatory deadlines, but it will further not enforce any penalties or fines against U.S. citizens or domestic reporting companies or their beneficial owners after the forthcoming rule changes take effect either. The Treasury Department will further be issuing a proposed rulemaking that will narrow the scope of the rule to foreign reporting companies only. Treasury takes this step in the interest of supporting hard-working American taxpayers and small businesses and ensuring that the rule is appropriately tailored to advance the public interest.
UPDATE ON CORPORATE TRANSPARENCY ACT REQUIREMENTS:
On Tuesday, December 23rd, 2024 the Fifth Circuit Court of Appeals reversed the USDC (E.D. Texas) decision granting a nationwide preliminary junction halting enforcement of the Corporate Transparency Act (CTA). All nonexempt reporting companies must comply according to the newly released deadlines below.
In response to this decision, the U.S. Department of Treasury’s Financial Crimes Enforcement Network (“FinCEN”) has indicated that reporting companies may need additional time to comply given the period when the preliminary injunction had been in effect, and has extended the reporting deadline as follows:
Reporting companies that were created or registered prior to January 1, 2024, have until January 13, 2025, to file their initial beneficial ownership information reports with FinCEN. (These companies would otherwise have been required to report by January 1, 2025.)
Other timelines based on business creation or registration:
- Reporting companies created or registered in the United States on or after September 4, 2024, that had a filing deadline between December 3, 2024 and December 23, 2024, have until January 13, 2025 to file their initial beneficial ownership information reports with FinCEN.
- Reporting companies Reporting companies created or registered in the United States on or after December 3, 2024 and on or before December 23, 2024 have an additional 21 days from their original filing deadline to file their initial beneficial ownership information reports with FinCEN.
- Reporting companies Reporting companies that are created or registered in the United States on or after January 1, 2025 have 30 days to file their initial beneficial ownership information reports with FinCEN after receiving actual or public notice that their creation or registration is effective.
If you have not already registered, you must do so immediately to avoid the heavy fines ($500 per day) and other potential penalties following the deadline.
- Follow this link to go to the Financial Crimes Enforcement Network (FinCEN) website for more information and to complete the BOI.
- Follow link to view the presentation by Dr. Scott Munsterman for more information regarding the Corporate Transparency Act.
The primary purpose of this webinar is for the Corporate Transparency Act for ALL LLC companies to report ownership. As of Jan. 1, 2024, many businesses will be required to report beneficial ownership information to the Financial Crimes Enforcement Network (FinCEN) to identify those who directly or indirectly own or control the company. This requirement stems from the enactment of the Corporate Transparency Act (CTA) passed with the National Defense Authorization Act for Fiscal Year 2021.
Beneficial Ownership Information Reporting | FinCEN.gov
The reporting requirements generally are applicable to small corporations, limited liability companies (LLCs) and other similar entities that:
- have 20 or fewer full-time employees; and
- filed federal income taxes in the previous year demonstrating $5 million or less in gross receipts or sales.
He will cover a couple of ICD-10 modifications as well, but primary purpose is the CTA
Click Here To View Webinar
Click Here To View PDF Notes
** All material presented on this website from third party sources, or otherwise, is intended for general informational purposes only since the services of a competent professional should be sought for any specific legal or other need. No attorney-client relationship is intended to be created by contacting this website or any individuals associated with this website.
